
What Is the Nuss Procedure?
The Nuss Procedure is a minimally invasive surgical technique used to correct pectus excavatum (sunken chest). Developed in 1987 by Dr. Donald Nuss at Children's Hospital of The King's Daughters in Norfolk, Virginia, it has become the preferred surgical treatment for many patients with moderate to severe chest wall deformities.
Dr. Barry LoSasso trained directly with Dr. Donald Nuss and has performed more than 1,500 Nuss Procedures in children, adolescents, and adults. As the director of a designated Center of Excellence for Pectus, Dr. LoSasso specializes in the evaluation and treatment of chest wall deformities and is recognized for his extensive experience with both pediatric and adult patients.
How Does the Nuss Procedure Work?
The Nuss Procedure is performed through small incisions placed on the sides of the chest. Using specialized instruments and thoracoscopic guidance, one or more curved stainless-steel bars are positioned beneath the sternum.
Once in place, the bar is carefully rotated, elevating the breastbone and restoring a more normal chest contour. The bar is secured to the chest wall to maintain correction while the chest remodels around its new shape.
Depending on the patient's age, anatomy, and severity of the deformity, one or more bars may be required to achieve the best possible result.
Nuss Procedure for Children and Adolescents
The ideal age for surgical correction is typically between 13 and 16 years, when the chest wall remains flexible but sufficient growth has occurred to achieve a durable correction.
Many patients begin noticing symptoms during adolescence, including:
Shortness of breath during exercise
Reduced athletic endurance
Chest discomfort
Fatigue
Self-consciousness regarding chest appearance
Although pectus excavatum is rarely life-threatening, it can significantly affect physical performance, posture, self-confidence, and overall quality of life.
Nuss Procedure for Adults
Dr. LoSasso is among a select group of surgeons with extensive experience performing the Nuss Procedure in adults.
Many adult patients either did not have access to treatment when they were younger or chose not to pursue surgery until later in life. While adult chest walls are generally less flexible than those of adolescents, advances in surgical techniques and pain management have made the Nuss Procedure a safe and effective option for carefully selected adult patients.
Patients frequently report improvements in exercise tolerance, breathing capacity, posture, and confidence following correction.
Recovery After Surgery
Recovery is an important part of the treatment process. Dr. LoSasso works closely with a specialized pain management team to provide comprehensive care before, during, and after surgery.
Modern pain-control strategies, early mobilization, and structured rehabilitation protocols help patients return to normal activities as safely and comfortably as possible. Every patient receives individualized guidance throughout the recovery process.
Nuss Bar Removal
The final stage of treatment is removal of the Nuss bar or bars after the chest wall has permanently remodeled into its corrected position.
For most patients, bar removal is performed approximately three years after the initial procedure. The timing may vary based on age, growth, and the severity of the original deformity.
Bar removal is typically an outpatient procedure performed under general anesthesia, allowing patients to return home the same day. Recovery following bar removal is generally much easier and less uncomfortable than the original corrective surgery.
Continuity of Care Matters
Dr. LoSasso believes that, whenever possible, the surgeon who performs the initial Nuss Procedure should also perform the bar removal. Continuity of care provides familiarity with the patient's anatomy, surgical history, and treatment plan, helping to ensure the safest and most effective outcome throughout every stage of the pectus repair process.
Why Choose Dr. Barry LoSasso?
Trained directly by Dr. Donald Nuss, inventor of the Nuss Procedure
More than 1,500 Nuss Procedures performed
Treating pectus patients since 1999
Extensive experience treating both pediatric and adult patients
Designated Center of Excellence for Pectus
Comprehensive care from initial evaluation through bar removal
For patients and families considering treatment for pectus excavatum, Dr. LoSasso provides expert evaluation, personalized treatment planning, and experienced surgical care at every step of the journey.
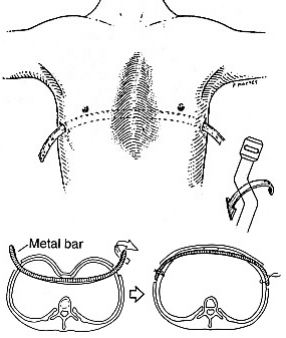
Metal Bar Placement
Webinar Recording: Removing the Pectus Excavatum Bars
“Dr. LoSasso and his team are truly amazing. We are so grateful for their caring demeanor, professional care and friendly atmosphere at their practice.”
— Michael
